Studies in development
ENTRAP
ENTRAP
ENTRAP
Regenerating nerves are swollen and recovery may slow due to extrinsic compression. The ENTRAP pilot is evaluating the reliability of clinical signs of nerve compression and the response to release of distal compression points after proximal nerve injury.
NEON
ENTRAP
ENTRAP
NEON is a collaboration with the RSTN, NDORMs at Oxford and the UEA. Digital nerve repair outcomes are of functional uncertainty with comparable neuroma rates with non-repaired nerves. the project is part of the NIHR HTA call for a UK multi-centre study in digital nerve repair. Dominic Power is a co-applicant and lead at UHB.
MONTHS
ENTRAP
MONTHS
MONTHS: Motor Outcomes following Nerve Transfer and Histopathological correlation Study. The MONTHS is a pilot feasibility study that is evaluating functional outcome after nerve transfer and will correlate with residual axon density after nerve injury.
WRAP
UNDER-Study
MONTHS
WRAP: Wrapping of nerves during Revision surgery for the Alleviation of Pain. The WRAP pilot started at UHB in 2016 and is evaluating pain outcomes and function after revision nerve decompression surgery.
UNDER-Study
UNDER-Study
UNDER-Study
UNDER-Study: Ulnar Nerve Decompression versus medial Epicondylectomy Study pilot.
The pilot is a establishing the validity of the PRUNE score as a PROM for use in a future RCT in cubital tunnel surgery. Please get in touch is you want to be involved in the pilot study.
Site Content
PAIN-Pilot
Allograft M+M
Allograft M+M

Allograft M+M
Allograft M+M
Allograft M+M

PANIC
Allograft M+M
I HaND +

I HaND +
I HaND +
I HaND +

P3NS
I HaND +
PAMTraC

PAMTraC
I HaND +
PAMTraC

RHINO - P
Want to become a researcher?
RHINO - P

Tomas Madura is leading on the RHINO - P pilot study examining the effect of ibuprofen on outcomes after peripheral nerve injury repair. Grant funding support is in place for the pilot study and potential collaborating centres for the main study are undergoing feasibility evaluation.
PICO - 7Y
Want to become a researcher?
RHINO - P

The PICO 7Y is a multi-centre commercially funded study assessing the PICO system in wound management following breast surgery. The HaPPen team are facilitating site adoption at UHB.
Want to become a researcher?
Want to become a researcher?
Do you have a commercial trial you want to run?

Where do I start?
Do you have a clinical problem you want to solve?
What about an idea for a clinical trial?
Perhaps you don't know how to proceed?
Contact the HaPPeN team and we can help you develop your idea and engage with potential collaborators.
Do you have a commercial trial you want to run?
Are you looking for collaborators to join your trial in the UK?
Do you have a commercial trial you want to run?

If you are a commercial organisation and want to run a trial in Hand, Plastics or Peripheral Nerve Surgery, then contact the HaPPeN team to discuss how we can help with trial design, establishing multi-centre partners and facilitation of trial delivery in the UK.
Are you looking for collaborators to join your trial in the UK?
Are you looking for collaborators to join your trial in the UK?
Are you looking for collaborators to join your trial in the UK?

Are you a researcher who is looking to identify potential collaborators?
The HaPPeN team can help to develop links with our established research partners across the UK and potential nerve surgery collaborators through the UK PN-CRN.
Need advice on trial design or structuring a research strategy?
Are you looking for collaborators to join your trial in the UK?
Are you looking for collaborators to join your trial in the UK?

For start-up companies with a new device or technology and limited trial experience, contact the HaPPeN team who can advise on trial design and cost-effective research strategy and help you develop a robust evidence base. The HaPPen team are working with partners in the UK, Europe and the USA on developing research for new biomedical technologies.
ENTRAP
ENTRAP: Efficacy of distal Nerve Release After Proximal injury
ENTRAP is a pilot feasibility study evaluating the rate of nerve regeneration after proximal continuity injury, the clinical signs associated with distal entrapment and the response to surgical release.
The pilot study is being conducted with at University Hospitals Birmingham.
The study is registered with C-ARMS and is evaluating clinical efficacy of decompression in upper limb and lower limb nerve injuries following trauma or iatropathic injury.


NEON
NEON
The NEON study is a collaboration through the NDORMs team at Oxford, UEA, UHB and the RSTN to develop a multi-centre trial in digital nerve injury in response to the NIHR HTA call.
The team have developed research protocol to evaluate the efficacy of digital nerve repair in terms of patient sensation, function, satisfaction and complications in addition to health economics around the intervention. The preliminary work includes a systematic review on outcomes after digital nerve repair published in March 2019 in BMJOpen.
The lead applicant is Professor Abhilash Jain, with Professor Christina Jeroch Herold, Professor David Beard and Dominic Power.
Professor Jain attended the first UK PN-CRN meeting at the Institute of Translational Medicine in Birmingham, hosted by the HaPPeN team in April 2018 where he presented the concept for the study and a consensus group helped to define the specific research question and feasibility of multi-centre recruitment in the UK.
Learn More
The NEON study is being developed in collaboration with the NDORMs team at Oxford, The academic department of rehabilitation research at the University of East Anglia, the RSTN and Dominic Power in the HaPPeN team.
months
MONTHS: Motor Outcomes after Nerve Transfer Histopathological correlation Study
Nerve transfer study is established as a reconstruction option for the management of paralysis. In complete nerve injury the proximity of nerve transfer to the motor point allows early functional restoration in otherwise non-reconstructable nerve root avulsion injuries, salvage of late presenting cases and when proximal reconstruction of a nerve injury has failed to achieve useful functional recovery.
The application of the technique to other causes of paralysis including tetraplegia, degenerative spinal motor radiculopathy and post neuritis paralysis is controversial.
The MONTHS study is a pilot evaluation of nerve transfer in paralysis reconstruction with correlation of clinical outcomes and axon counts within the donor and recipient nerves harvested at the time of transfer.
Learn More
Nerve transfer may restore function to paralysed muscles, however the scope of the technique is not fully understood. The aim of the pilot is to develop a study evaluating motor outcome with correlation with the extent of axonal degeneration evidenced through donor and recipient nerve analysis when harvested at the time of transfer.

WRAP
WRAP: Wrapping of nerves during revision surgery for the Alleviation of Pain
Neurostenalgia is a painful tether or compression syndrome due to scar and restricted glide of the affected nerve. Revision decompression and neurolysis may improve pain, however recurrent scar may result in a temporary or resolution of symptoms. the WRAP pilot is a study evaluating clinical functional and pain outcomes after wrapping scarred nerves with the AxoGuard TM nerve protector during revision surgery.
The AxoGuard is a layered porcine extracellular matrix that can be positioned around injured or scarred nerves. Revascularisation allows restoration of nerve glide.
The study is registered with C-Arms and the utility and safety data was published in the Journal of Musculoskeletal Surery and Research in January 2019. The efficacy data for revision cubital tunnel will be presented at the IFSSH meeting in Berlin, June 2019. The efficacy data for cubital tunnel revision and carpal tunnel revision will be published in 2019.
The aim of the pilot study is to inform the development of a future multi-centre study in this area including health economics data.
No funding support has been received for the pilot WRAP study.
Learn More
Neurostenalgia is a painful tether or compression of a nerve due to scar. There are several commercial wrapping barriers for use in revision nerve surgery for prevention of recurrent scar. The WRAP pilot is measuring functional recovery and pain relief following use of a collagen nerve wrap.
UNDERStudy
UNDERStudy: Ulnar Nerve Decompression versus medial Epicondylectomy Randomised Study
Failed cubital tunnel surgery is a challenging problem. Ulnar neuropathy has both compression and tension components to the syndrome. Simple decompression is the most common procedure for cubital tunnel syndrome and dresses only the compression component and in some situations can result in new symptoms due to nerve subluxation at the elbow during elbow flexion.
Revision surgery can include simple decompression, neurolysis and wrapping or the nerve, subcutaneous and sub muscular transposition. Medial epicondylectomy is a technique that addresses both compression and tension, however there are additional potential complications when compared to simple decompression.
There is no consensus on the optimum strategy for management. A systematic review on cubital tunnel surgery was completed by Eva O'Grady, the HaPPeN Research Fellow in 2017. A survey of UK practice amongst hand surgeons demonstrated variation in practice and established that medial epicondylectomy is rarely performed in primary surgery.
The peripheral nerve team at UHB use the medial epicondylectomy technique in revision surgery and in some primary surgery cases where there is subluxation or subjective tension following decompression.
The aim of the pilot study is to collect preliminary outcome data using the PRUNE score which os a validated PROM fr cubital tunnel surgery. The pilot will evaluate the feasibility for a future RCT and will establish normal responsiveness following medial epicondylectomy.
The study is registered with C-Arms at UHB and has been collecting baseline PROM data since 2016.
Learn More
The PRUNE is a validated tool for the measurement of outcome after surgery for ulnar nerve compression at the elbow. The Pilot study is collecting feasibility and outcome data to establish whether the PRUNE can be used as the primary outcome measure for a future RCT in cubital tunnel surgery.
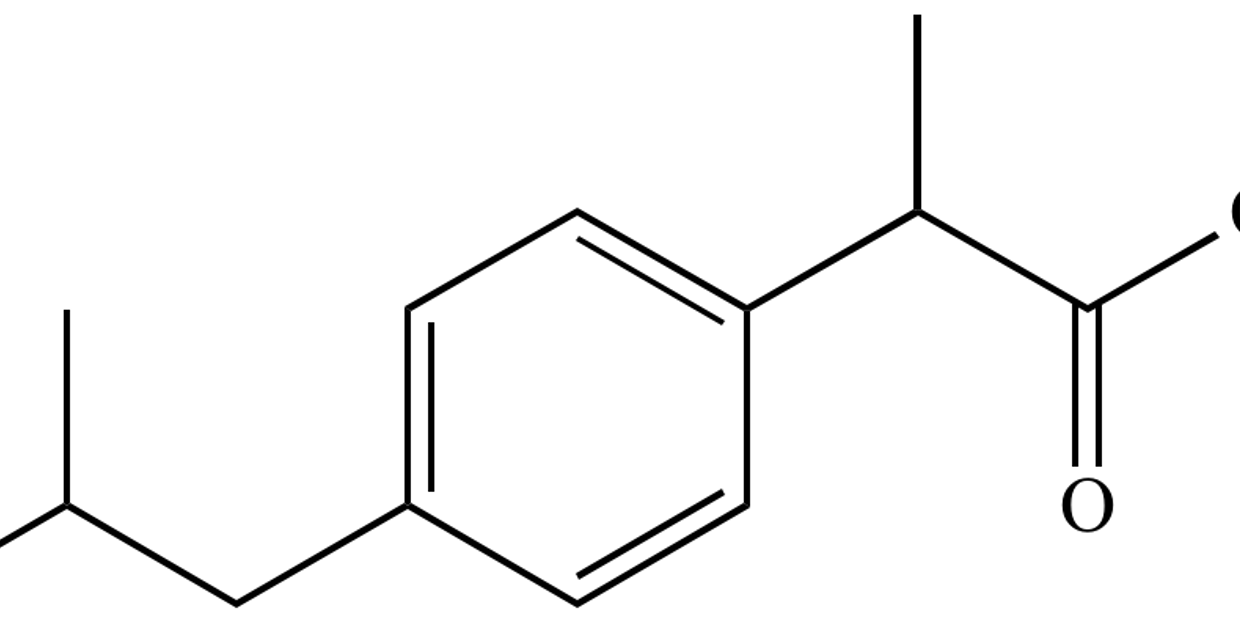
RHINO-P
Rhino-P: Pilot study of Rho kinase inhibition in nerve repair outcomes
Tomas Madura is the lead investigator for this pilot study investigating the use of ibuprofen in peripheral nerve repair.
The study pilot has received grant funding and the protocol is being developed. A feasibility study in 2018 established potential research partners for recruitment across the UK for the multi-centre trial roll-out.
For more information or to discuss collaboration opportunities, please contact the HaPPeN team using the "contact us" link at the below.
Learn More
Rhino-P is a pilot study that is being developed to evaluate efficacy of ibuprofen in nerve recovery following repair or complete transection injuries.
Contact Us
Better yet, see us in person!
We love our customers, so feel free to visit during normal business hours.
HaPPeN Research Network
Hours
Open today | 09:00 – 17:00 |
